Seems to be pot luck... if you are making an appointment some pharmacies offer a choice. If it is say your GP or an MVC you don't seem to get a choice.Is there a choice available? I'm due for my second booster soon.
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
The safety of the new vaccine
- Thread starter Brendan Burgess
- Start date
- Status
- Not open for further replies.
Yeah, the vaccines seem to reducing severity of illness if not the incidenceLook at the death rates in comparison to infections. There are much less deaths.
Our current daily cases are above two of our three previous peaks, but our deaths are at all time low.
Vaccine seems like a likely cause for that.
WaterWater
Registered User
- Messages
- 485
I am also hearing this. Family members that had no problems with the first three jabs are getting flu like symptoms after the second booster. Have they changed the formula I wonder?A friend had no problems with his first two vaccinations nor with his booster. He went for his second booster recently and was very unwell, with flu like symptoms for 24 hours. Is this common?
It's probably that they got one vaccine originally and are now getting Moderna which seems to trigger a stronger immune reaction - at the cost of tough immediate short term side effects. I think I read something to the effect Moderna has more mRNA bang for buck in it than Pfizer also.I am also hearing this. Family members that had no problems with the first three jabs are getting flu like symptoms after the second booster. Have they changed the formula I wonder?

Moderna vs. Pfizer: Is There a “Best” mRNA Vaccine?
Both of the mRNA vaccines available in the US are highly effective against severe COVID-19, but recent studies suggest that Moderna’s elicits a stronger immune response and might be better at preventing breakthrough infections.
WaterWater
Registered User
- Messages
- 485
I would prefer one of the original ones, like I had before. I don't want to be sick from a vaccine.It's probably that they got one vaccine originally and are now getting Moderna which seems to trigger a stronger immune reaction
Bronco Lane
Registered User
- Messages
- 523
I am a two Astrazeneca and a Pfizer booster recipient. I don't wish to get the Moderna as a booster. Read too many reports of people getting or having their tinnitus increasing after the Moderna.
Can I have a choice of booster?
Can I have a choice of booster?
Ask your GP or Pharmacy which one they give. I don't know whether they are still running Vaccine Centres. You can just decline if it's not the one you want and try to make a different appointment. I've had 2 x Pfizer and a Moderna chaser . . I've had the Covid twice . . I'm done with vaccines.
Bronco Lane
Registered User
- Messages
- 523
I was only discussing this with the other half this morning. We each have been jabbed 3 times but with still got Covid albeit a low dose.I've had 2 x Pfizer and a Moderna chaser . . I've had the Covid twice . . I'm done with vaccines.
Everyone says the same thing...."but it would have been much worse if you hadn't been vaccinated".
Why would you boost your immunity to a strain that is no longer in circulation i.e. Wuhan ? I don’t understand how a booster can offer protection when many mutations have occurred.
Would you take a two year old flu jab? Personally I would not. Neither would it be offered to me as they are updated annually to match the top 3 or 4 variants in circulation. Otherwise they don’t give protection. Occasionally they don’t get the cocktail correct. A few years back I got Aussie flu as it wasn’t included in the jab.
Would you take a two year old flu jab? Personally I would not. Neither would it be offered to me as they are updated annually to match the top 3 or 4 variants in circulation. Otherwise they don’t give protection. Occasionally they don’t get the cocktail correct. A few years back I got Aussie flu as it wasn’t included in the jab.
Why would you boost your immunity to a strain that is no longer in circulation i.e. Wuhan ? I don’t understand how a booster can offer protection when many mutations have occurred.
Would you take a two year old flu jab? Personally I would not. Neither would it be offered to me as they are updated annually to match the top 3 or 4 variants in circulation. Otherwise they don’t give protection. Occasionally they don’t get the cocktail correct. A few years back I got Aussie flu as it wasn’t included in the jab.
It's not the same situation.
The covid vaccines also worked very effectively against Alpha and Delta variants in terms of protection against infection.
The booster boosts your immunity against coronavirus strains including Omicron. It triggers neutralizing antibodies against Omicron, though fewer than it triggered for other variants. Omicron has more mutations than the other strains but not so many that if vaccinated your immune system doesn't recognise it as covid.
And these antibodies wane.
Importantly against all strains it provides durable protection against severe covid - through your immune system T cells.
This protection wanes more slowly and the seems to wane faster in older people.
So that's why a booster of the same vaccine for covid can still be beneficial - more so for those who need the boost or if you are dealing with vulnerable people, then when boosted you are less likely to get infected.
A study of triple vaccinated people in Qatar versus Omicron showed a 52% reduction in cases, although this wanes after 4 months.
Whereas if you get an influenza A strain in the flu vaccine that is a mis-match to the strains, there doesn't appear to be any immune benefit.
There are some indications that influenza B protection is more widespread \ less specific - it hits children hardest. So a 2 year old flu jab with influenza B in it would still be beneficial.

Should you wait for an Omicron vaccine—or get your next booster now?
With Omicron subvariant BA.5 on the rise, many Americans are debating how best to protect themselves. Here's what experts say.
Studies found that COVID-19 vaccines elicit T cells that recognize the Omicron variant despite the many mutations in its spike protein.
The vaccines were designed to teach the immune system to recognize a key part of the spike protein. But they were developed using the initial SARS-CoV-2 spike protein. Studies have found that antibodies generated by these vaccines don’t recognize their targets as well in heavily mutated variants like Omicron.
They observed substantially fewer memory B cells and neutralizing antibodies in the blood of people 6 months after vaccination. Memory B cells help to quickly produce antibodies against previously encountered viruses or other pathogens. Having fewer neutralizing antibodies increases the risk of “breakthrough” infections—when vaccinated people are reinfected.
In contrast to antibodies, the team found that T cell responses from the vaccines recognized all variants, including Delta and Omicron. The majority of T cell responses remained effective against Omicron. Six months after vaccination, 84% of CD4+ (helper) T cell responses and 85% of CD8+ (killer) T cell responses against Omicron remained the same compared to early variants...
Despite reduced antibody responses against the variants, T cells serve as a second line of defense. This may help to explain why Omicron infections, while easily spread, are less likely to lead to severe disease in fully vaccinated people.
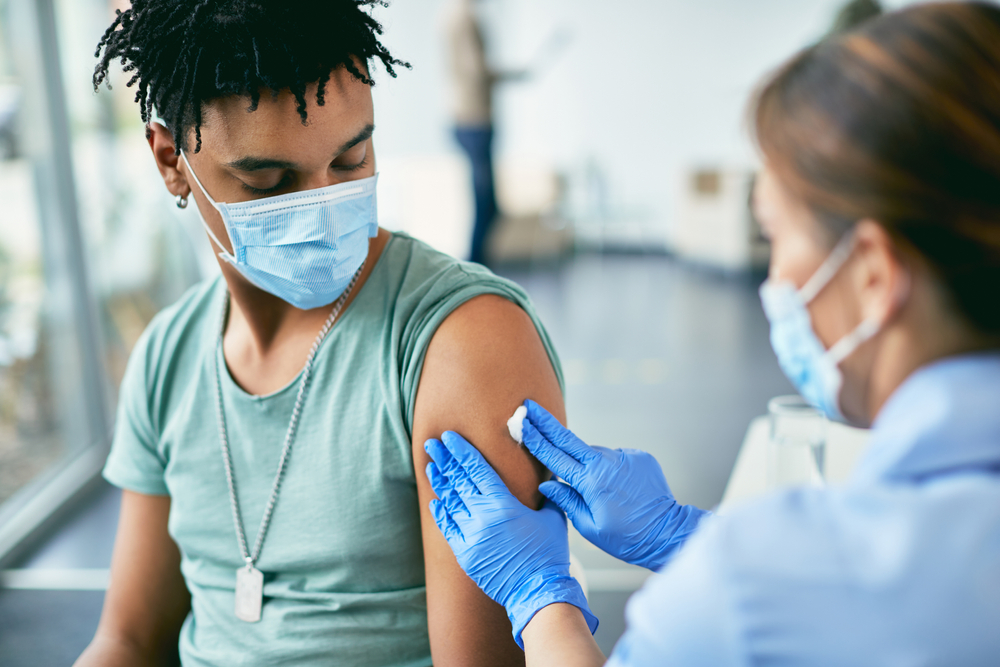
COVID-19 vaccines induce immune response to Omicron
Studies found that COVID-19 vaccines elicit T cells that recognize the Omicron variant despite the many mutations in its spike protein.
Last edited:
I had covid around four months ago. I had not been vaccinated at all. It was certainly an unpleasant few days but no where near as bad as Aussie flu which left me with pneumonia. I am over 50 and have an underlying condition. I recovered. I’m not convinced that a 2 year old booster has anything to add to my now measurable naturally acquired immunity to omicron. Naturally acquired immunity has not been discussed much by the media, but surely it must play an important role. I will take a flu jab though when it’s offered.
If you have recently had Omicron, why would you be so concerned about an Omicron specific booster?I had covid around four months ago. I had not been vaccinated at all. It was certainly an unpleasant few days but no where near as bad as Aussie flu which left me with pneumonia. I am over 50 and have an underlying condition. I recovered. I’m not convinced that a 2 year old booster has anything to add to my now measurable naturally acquired immunity to omicron. Naturally acquired immunity has not been discussed much by the media, but surely it must play an important role. I will take a flu jab though when it’s offered.
Rather strange questions.
Actually the booster you should want is a non-Omicron one, as effectively you have already been vaccinated v Omicron.
You were probably rather lucky you got Omicron unvaccinated rather than the earlier strains.
Natural acquired immunity wanes also, although based on this study Omicron it wanes more slowly v Omicron for naturally acquired immunity.
The headline refers to antibody immunity v protection.
Protection against severe covid is more long lasting for both types.
For those with no history of vaccination, SARS-CoV-2 infection during a prior-variant wave appeared to provide about 50 percent protection against symptomatic infection during the omicron wave, and this “natural immunity” was associated with almost the same degree of protection even a year after infection.
The combination of prior, full vaccination and prior infection was maximally protective: Individuals with prior infection and three doses of either mRNA vaccine were, overall, nearly 80 percent protected from symptomatic infection during the omicron wave.
Qatar Omicron-Wave Study Shows Slow Decline of Natural Immunity, Rapid Decline of Vaccine Immunity
A recent Pfizer or Moderna mRNA-vaccine booster provided good but temporary protection against infection by the SARS-CoV-2 omicron variant.
This is what happened when Omicron hit Hong Kong - older demographic without immunity from either vaccines or previous infection.
Even if Omicron is less severe, it is more infectious. IN the numbers game of hospital capacity, without vaccines, it is major threat to capacity.

 www.cidrap.umn.edu
www.cidrap.umn.edu
Even if Omicron is less severe, it is more infectious. IN the numbers game of hospital capacity, without vaccines, it is major threat to capacity.

Study sheds light on death spike in Hong Kong COVID-19 surge
An Omicron spike in Hong Kong with high mortality may be due to low vaccine uptake in older people.
Vaccines can cause myocarditis. Long covid can put you at risk of developing cardiac issues. Pre covid there were heart issues emerging with athletes.Spent a week on a ward with 4 men in 30s and 40s with heart issues. Not what I was there for. Also hearing this from somebody who works in health profession. What has caused all these heart conditions in young men ?
None of these lads had long convid. One was blaming the booster !Vaccines can cause myocarditis. Long covid can put you at risk of developing cardiac issues. Pre covid there were heart issues emerging with athletes.
None of these lads had long convid. One was blaming the booster !
It is possible, although such severe adverse effects are less likely with a booster dose (assuming original vaccine was mRNA):
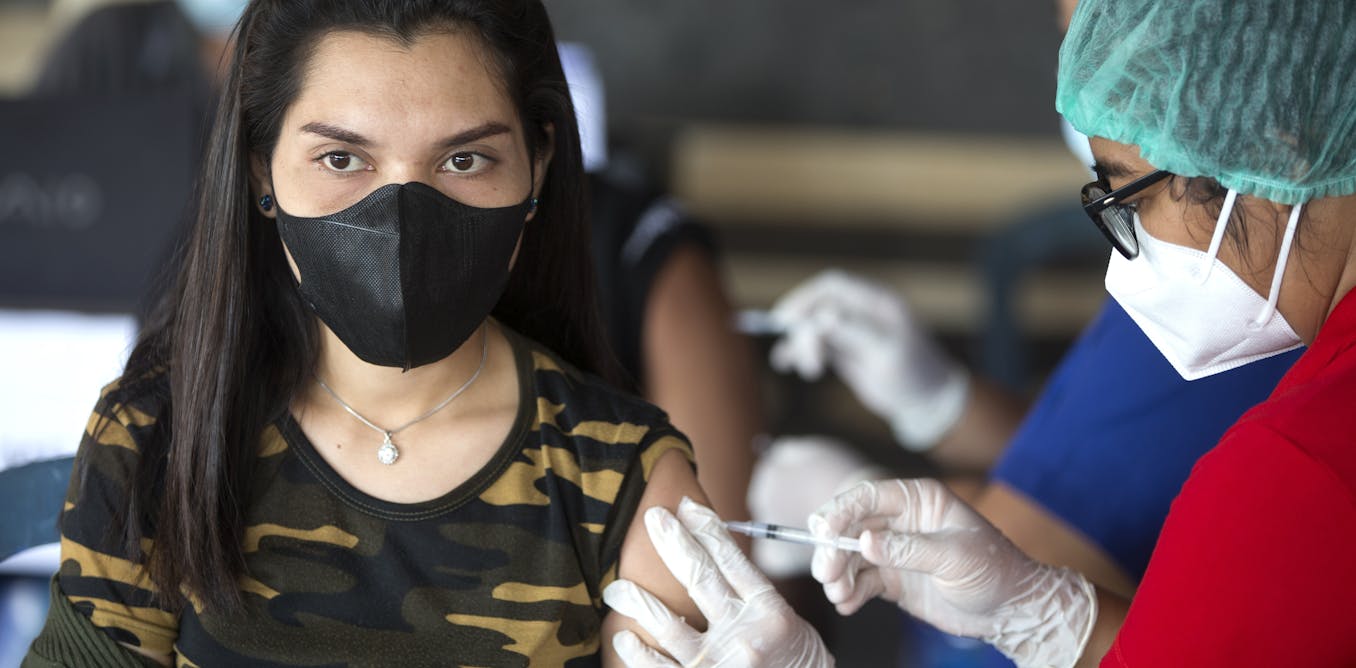
Do COVID boosters cause more or fewer side effects? How quickly does protection wane? Your questions answered
Fewer people reported needing to miss work after their booster, compared to their second dose.
 theconversation.com
theconversation.com
How many would there have been pre-covid? Is it higher or lower now? A single random experience is not indicative of anything.Spent a week on a ward with 4 men in 30s and 40s with heart issues. ... What has caused all these heart conditions in young men ?
The increasing prevalence of heart disease in younger adults has been a concern for some time.
It's easy to blame a booster for early heart issues while continuing with a poor diet and little or no exercise.
I've developed problems eating gluten. I blame electric cars. Before there were electric cars I'd no problem. Because I just think* correlation does actually equal causation.How many would there have been pre-covid? Is it higher or lower now? A single random experience is not indicative of anything.
The increasing prevalence of heart disease in younger adults has been a concern for some time.
It's easy to blame a booster for early heart issues while continuing with a poor diet and little or no exercise.
*"Just Thinking" means holding a view on a topic without examining the data or reading expert opinions etc.
- Status
- Not open for further replies.